Spotlight on Female Reproductive Health
We don't talk about this enough.
Despite our hyper-sexualized society, female reproductive health often gets swept under the rug. It can be uncomfortable to talk about, either in a social context or with a health professional, and it's certainly something that isn't especially fun to get checked out for.
But ladies, our sexual parts are just as important a part of our health as any other area of the body, so let's have a chat.
Endometriosis
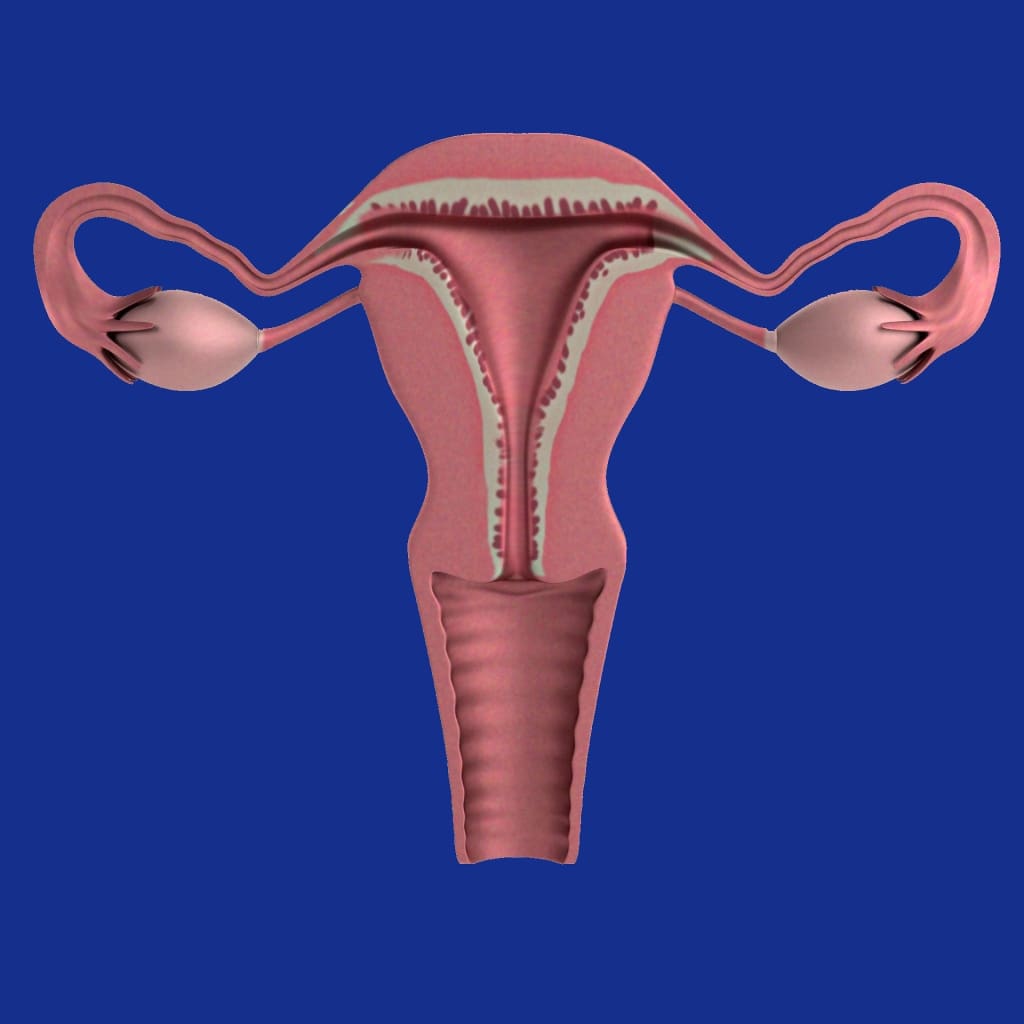
Every month, our uterus builds up an endometrial lining to prepare for a fertilized egg, and our period involves the shedding of this lining. Endometriosis is a condition where this endometrial tissue spreads out beyond the uterus. It can affect the ovaries, fallopian tubes, and other areas of the pelvis.
Endometriosis can cause significant pelvic pain, which is usually worse during menstrual periods. There can also be pain with sex or bowel movements. There can be heavy bleeding during and between periods. Fertility can be negatively affected.
There are several different strategies that may be involved in making a diagnosis. The first is a pelvic exam by your doctor. An ultrasound can determine whether any cysts have formed as part of the endometriosis. MRI imaging gives a high level of detail, and a laparoscopy involves inserting a small camera through your abdominal wall.
Hormones may be used to suppress the symptoms of endometriosis, although this isn't a cure. Surgical treatment can involve laparoscopic removal of the endometrial tissue in the pelvis, but this is not a permanent fix. A more extreme option is surgical removal of the uterus, and often the ovaries as well.
Polycystic Ovary Syndrome (PCOS)
This involves the formation of cysts in the ovaries. Menstrual cycles become irregular, with fewer periods than normal. Periods may involve heavy bleeding. There may be elevated levels of androgens (male hormones), causing acne and increased facial and body hair growth.
PCOS can cause infertility and miscarriage. It may increase the risk for diabetes, high cholesterol, sleep apnea, and uterine cancer. It is linked to mental health disorders like depression, anxiety, and eating disorders. Being overweight can worsen PCOS symptoms.
There isn't a specific test for PCOS, but diagnosis may involve a pelvic exam by your doctor, bloodwork, and an ultrasound.
Hormonal treatment may be used to regulate the menstrual cycle and decrease other symptoms. Hormonal agents may also be used to stimulate ovulation. Spironolactone is an anti-androgen that is sometimes used to manage hair growth.
Pelvic Inflammatory Disease (PID)
PID infection involves the female reproductive organs. It often begins with a sexually transmitted infection (STI) in the vagina, (e.g. chlamydia or gonorrhea) that moves upwards to affect other parts of the reproductive system.
It's often asymptomatic, but it can cause fever, abdominal pain, and foul-smelling vaginal discharge.
The best prevention is safer sex practices with a barrier method. If symptoms of an STI develop, treatment should be sought promptly to prevent the STI from developing into PID. Douching kills healthy bacteria in the vagina, so this should be avoided.
Complications of PID include infertility, ectopic (tubal) pregnancy, abscesses, and chronic pelvic pain.
Diagnosis is done by pelvic exam and blood and urine tests. Ultrasound or laparoscopy may also be used.
Treatment involves antibiotics, either oral or intravenously depending on how serious the infection is. The sexual partner should be treated as well to avoid reinfection.
Vaginismus
Vaginismus involves the involuntary, reflexive clenching of the vaginal muscles. This can make it difficult and painful or impossible to have sexual intercourse, have a pelvic exam, or even insert a tampon.
There is often a complex interplay of factors that contribute toward the development of vaginismus. Sexual activity may be desired, but the extreme pain and/or inability to relax the vaginal muscles enough to allow penetration can be highly mentally distressing.
Vaginismus can be difficult to manage. Strategies that may help include physiotherapy to work on muscle control, and the use of dilators to gradually work up to tolerating something larger inside the vagina. It may also be helpful to see a therapist to work on the cognitive/emotional element.
A great first-hand source of info on this condition is Victoria Johnston's book Living with Vaginismus: Dealing with the World's Most Painful Pleasure.
Conclusion
These are just a few of the conditions that can affect women's reproductive health. It's important to know that whatever you might be experiencing "down there," other people are going through the same issues and it's a valid problem deserving of help. If something doesn't seem right, go see your health care provider. You (and your lady bits) are so worth it.
Sources
Mayo Clinic: Polycystic Ovary Syndrome
About the Creator
Ashley L. Peterson
Mental health blogger | Former MH nurse | Living with depression | Author of 4 books: A Brief History of Stigma, Managing the Depression Puzzle, Making Sense of Psychiatric Diagnosis, and Psych Meds Made Simple | Proud stigma warrior
Enjoyed the story? Support the Creator.
Subscribe for free to receive all their stories in your feed. You could also pledge your support or give them a one-off tip, letting them know you appreciate their work.






Comments
There are no comments for this story
Be the first to respond and start the conversation.