COVID-19 Vaccine for Transplant Patients: To Vaccinate or Not to Vaccinate?
Should an immunosuppressed organ transplant recipient get the COVID-19 vaccine?
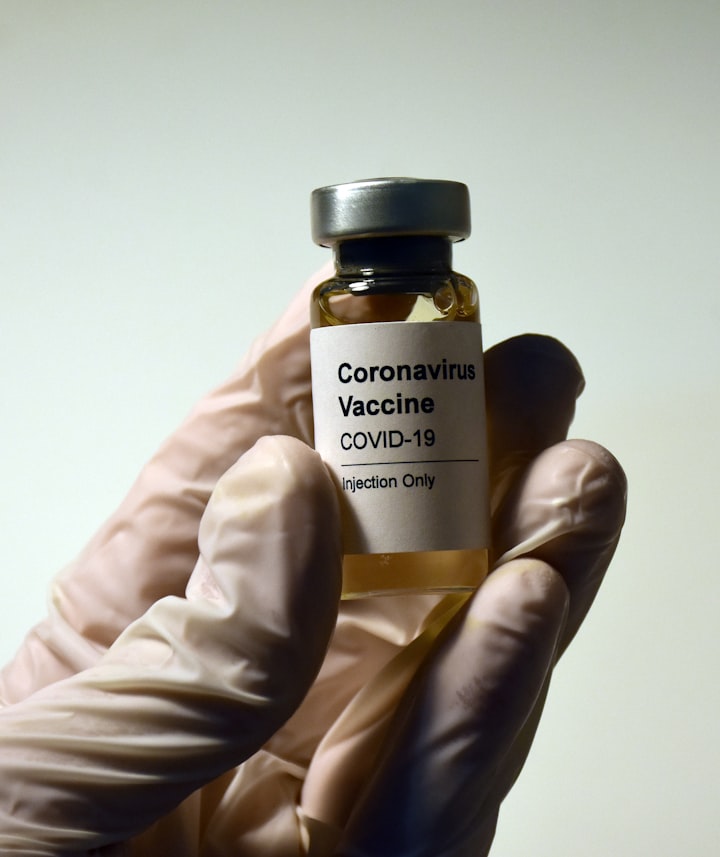
As a recent recipient of a set of new lungs, I am uber cautious about protecting myself from contracting COVID-19 coronavirus. Diagnosed with polymyositis, a rare autoimmune disease, I have become vulnerable to the world around me. So, I decided to do some research on available COVID vaccines to potentially protect myself from damaging my transplanted organs. What I discovered wasn't very promising for someone like me.
On the few transplant forums I’ve come across that discuss the fears of negative vaccination side effects, there have been reports of people showing signs of organ rejection. That scares me. After going through the ordeal of lung failure, waiting for a match, and undergoing an equally lifesaving and life-threatening surgery-- rejection is the last thing you want to worry about.
Luckily, I couldn’t find any official reports of organ rejection after receiving a COVID-19 vaccination. Hopefully, lives are not lost as a result. With 2.86M deaths worldwide, this pandemic has taken enough lives. I did find research on the recommendations for COVID-19 vaccines for transplant patients and immunosuppressed individuals.
“It is recommended that transplant recipients receive whatever vaccine may be available to them.” However, “transplant patients were excluded from the initial trials” and most studies only reveal how effective the COVID-19 vaccinations are for “general patient populations.” (VCU Health, 2021)
For healthy individuals or at least those who have healthy immune systems, the following are the reported effectiveness for the three available vaccines.
• Pfizer vaccine is 95% effective at preventing COVID-19 in general patient populations.
• Moderna vaccine is 94% effective at preventing COVID-19 in general patient populations.
• Johnson & Johnson vaccine is 85% effective at preventing severe COVID-19 in general patient populations.
For those individuals who the vaccines are effective, nearly 100% of them develop antibodies. (Johns Hopkins, 2021) Although there is no guaranteed predetermined amount of time the vaccine will remain effective, the range is typically eight months or more. This vaccine will likely have to be administered annually like the flu vaccine.
According to the CDC, “COVID-19 vaccination works by teaching your immune system how to recognize and fight the virus that causes COVID-19” protecting you from getting sick and possibly spreading the virus to someone else. Because of this, non-immunosuppressed individuals could do more for those around them by getting vaccinated.
It is helpful for individuals within the general patient population to get vaccinated to help protect the immunosuppressed and transplant recipients. That may be even more effective than people like me receiving the vaccine ourselves.
According to a recent Johns Hopkins study, only 17 percent of transplant recipients are reported to develop antibodies from the COVID-19 vaccine after their first dose. This was determined after transplant recipients received the most effective of the three vaccines, Pfizer and Moderna. Although the vaccines contain no live coronavirus, you’re likely to have a greater rate of exposure venturing out into the world to get the vaccine than actually being protected by it once it’s received.
It is said that “any degree of protection from this deadly disease is better than no protection.” However, 17 percent is hardly any protection and if there is no guarantee that rejection won’t be triggered, a double lung transplant recipient like myself is better off staying home.
Does hope cause people to make bad decisions or is that just a synonym for naivety? I don’t want to make a bad decision simply hoping that a COVID-19 vaccine will protect my new lungs. Just because someone suggests I trust the medicine without scientific evidence to support its effectiveness for someone like me, does not mean I should. In my opinion, receiving a vaccine now would be premature.
Until there is research to show that the benefits outweigh the risks, I think I should continue to leave my home only when necessary, double up on my masks, and frequently wash my hands. There just isn’t enough information available for organ transplant recipients to be certain of definite protection.
COVID-19 Vaccines Aren't Enough for Immunosuppressed.
If you’d like to see more from me, kindly give a coin of encouragement.
#RobinsDoOver
Resources:
COVID-19 vaccines and transplant patients: Is vaccination safe? Benefits of Getting a COVID-19 Vaccine COVID-19 Story Tip: Covid-19 Vaccines May Not Produce Sufficient Antibody Response in Transplant Recipients
About the Creator
Robin Jessie-Green
Temple University BA and AIU Online MBA Alumna.
Content Contributor for Medium, eHow, Examiner, Experts123, AnswerBag, Medicine-guides.com and various other sites spanning a decade.
Visit my Writing Portfolio to see what else I've written.






Comments
There are no comments for this story
Be the first to respond and start the conversation.