PRP Therapy for Arthritis: A Regenerative Treatment for Joint Pain
PRP Therapy Unleashed as a Cutting-Edge Solution for Arthritis
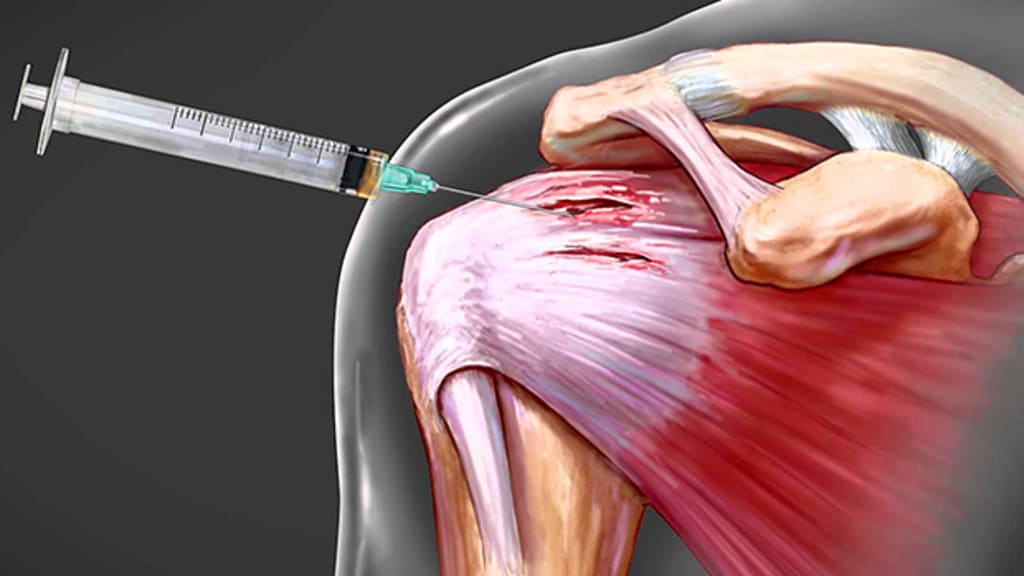
Arthritis is a common condition that affects millions of people worldwide. It occurs when the cartilage that protects the joints wears down over time, leading to pain, inflammation, and reduced range of motion. While arthritis cannot be cured, new advances in regenerative medicine are providing hope for long-lasting arthritis pain relief. One of the most promising treatments is platelet-rich plasma (PRP) therapy.
What is PRP Therapy?
PRP therapy utilizes injections of concentrated platelets extracted from the patient’s own blood to treat damaged joints and accelerate healing. r3stemcell has emerged as a leading provider of cutting-edge PRP treatments.
To prepare a PRP injection, a small sample of blood is drawn from the patient. This blood then undergoes a centrifuge process to separate and concentrate the platelets from other blood components. The platelets contain alpha granules that are abundant in growth factors and proteins essential for tissue regeneration and healing.
Once activated, the platelets release their growth factors which trigger localized inflammation and initiate the body’s natural healing response. The PRP injection introduces a high concentration of growth factors directly into the damaged joint, attracting stem cells that aid cartilage and tissue regeneration.
PRP therapy helps reduce arthritis pain and inflammation while potentially slowing the progression of osteoarthritis. It is an appealing treatment option because it utilizes the patient’s own blood and does not require surgery.
Understanding Arthritis
Arthritis encompasses over 100 rheumatic diseases that damage the joints and connective tissues, causing chronic inflammatory pain. The two most common types are osteoarthritis and rheumatoid arthritis.
Osteoarthritis
Osteoarthritis is a degenerative joint disease resulting from cartilage breakdown in the joints. It most often affects the knees, hips, hands, and spine. As the cartilage deteriorates, symptoms include:
- Joint pain, stiffness, and swelling
- Reduced flexibility and range of motion
- Bone spurs or loose bone fragments
- Joint instability and misalignment
While osteoarthritis cannot be reversed, PRP injections may help slow its progression and provide lasting pain relief by healing damaged cartilage.
Rheumatoid Arthritis
Rheumatoid arthritis is an autoimmune disorder where the immune system attacks healthy joint tissues. It causes painful inflammation and can damage cartilage, bones, and ligaments. Symptoms include:
- Stiff, tender, swollen joints
- Fatigue, fever, and weight loss
- Joint deformity or misalignment
- Low appetite, anemia
For some patients, PRP therapy may help reduce rheumatoid arthritis symptoms by decreasing inflammation and providing joint lubrication. However, results vary by individual.
The Role of Platelets in Healing
Platelets are colorless blood cells vital for clotting. Beyond their clotting function, platelets release growth factors essential for tissue and wound healing. Key growth factors in PRP include:
- Platelet-derived growth factor (PDGF): Stimulates cell growth and new blood vessel formation. Helps regenerate connective tissue.
- Transforming growth factor β (TGF-β): Regulates inflammation and supports cartilage regeneration. Also attracts stem cells.
- Fibroblast growth factor (FGF): Promotes tissue repair, angiogenesis, and stem cell migration.
- Vascular endothelial growth factor (VEGF): Stimulates new blood vessels and capillary growth to improve circulation.
- Epidermal growth factor (EGF): Activates tissue growth and accelerates epithelial tissue regeneration.
Introducing a concentrated dose of these growth factors via PRP therapy boosts the body’s natural healing abilities. The growth factors reduce inflammation, attract stem cells, stimulate new cartilage and tissue growth, and enhance circulation.
How PRP Therapy Reduces Arthritis Pain
For osteoarthritis patients, PRP injections aim to repair cartilage damage and lubricate joints. The injected platelets release growth factors that:
- Initiate anti-inflammatory processes to reduce joint swelling and pain
- Stimulate new cartilage growth and tissue regeneration
- Improve collagen production for tendon and ligament repair
- Attract stem cells to aid cartilage regeneration
- Increase joint lubrication and mobility
This combination of anti-inflammatory, regenerative, and lubricating effects provides ongoing pain relief. Patients report improved joint flexibility and a significant reduction in arthritis symptoms.
Is PRP Therapy Effective for Arthritis?
Numerous studies demonstrate PRP therapy safely reduces osteoarthritis pain and improves mobility without major side effects. A 2015 study in the American Journal of Sports Medicine found PRP provided rapid pain relief for mild knee osteoarthritis, and this pain relief lasted up to 2 years.
A 2019 meta-analysis of 10 high quality studies on knee osteoarthritis concluded PRP injections significantly decreased pain and increased function for up to 1 year. PRP outperformed hyaluronic acid injections.
While some patients experience immediate pain relief, it typically takes 4-6 weeks to feel the full effects. Most patients opt for 1-3 PRP treatments spaced 3-6 months apart for sustained benefits. Combining PRP with gentle physical therapy may further improve outcomes.
PRP therapy is less proven for rheumatoid arthritis but shows promise for reducing inflammation and severe joint pain. More studies are still needed. Always consult your doctor to see if PRP is right for your individual arthritis type and condition.
What to Expect During PRP Injections
Receiving PRP therapy is an outpatient procedure that takes less than 1 hour. Here is what to expect:
- A small blood sample (less than 60 mL) is collected from your arm.
- The blood spins in a centrifuge, separating and concentrating the platelets.
- Your joint area is sterilized and numbed with local anesthesia.
- Using imaging guidance, the PRP is injected directly into the arthritic joint(s).
- Bandages are applied and you can go home shortly after.
You may feel mild joint soreness for a few days post-injection as the growth factors initiate healing inflammation. Avoid strenuous activities for 1-2 weeks. Over-the-counter pain medication can provide relief.
PRP vs Stem Cell Therapy
- Like PRP, stem cell therapy is another promising regenerative treatment. It involves injecting stem cells from a patient’s own body to initiate healing.
- Key differences between PRP vs stem cells:
- PRP uses platelets and proteins from your blood. Stem cells come from fat or bone marrow.
- PRP signals local stem cells to migrate to the joint. Stem cell therapy directly injects stem cells.
- PRP takes less than 1 hour. Stem cell therapy is more invasive since cells must be harvested first.
- PRP costs around $1,000 per treatment. Stem cell therapy starts at around $5,000.
- Both reduce inflammation and may regenerate cartilage. More research is needed.
Providers like r3stemcell can advise whether PRP, stem cell therapy, or both used together are most suitable for your arthritis.
Takeaway: Give PRP a Try for Ongoing Arthritis Pain Relief
Countless osteoarthritis sufferers have found lasting pain relief from PRP injections. This cutting-edge, non-surgical treatment uses your body’s natural healing abilities to decrease joint inflammation and potentially regenerate damaged cartilage.
While results vary, many patients experience over a year of pain relief from just 1-3 PRP treatments. The procedure is safe, non-invasive, and more affordable than surgery. By reducing arthritis symptoms and joint damage, PRP therapy can help you reclaim your active lifestyle.
Consider scheduling a consultation with a reputable PRP provider like r3stem cell to see if you are a candidate. Though not a cure, PRP gives new hope to arthritis patients looking for safe, lasting relief from joint pain.





Comments
There are no comments for this story
Be the first to respond and start the conversation.