The Vascular Effects of Hormonal Changes in Women
Understanding the Link to Varicosity

Did you know that hormonal fluctuations in women can lead to the development of varicose veins?
Varicose veins are not just a cosmetic concern. They can cause discomfort, pain, and even lead to serious health complications. Understanding the role hormones play in the development of varicose veins can help women make informed decisions about their health and well-being.
A Quick Peek into the World of Hormones and Vascular Health
Hormones are chemical messengers that regulate various physiological processes in our bodies. For women, hormonal fluctuations are a natural part of life, occurring throughout the menstrual cycle, pregnancy, and menopause. These fluctuations can have a significant impact on vascular health, including the development of varicose veins.
Research has shown that hormones such as estrogen and progesterone play a crucial role in maintaining the elasticity and strength of blood vessels. However, fluctuations in these hormone levels can weaken the vein walls and valves, leading to the development of varicose veins.
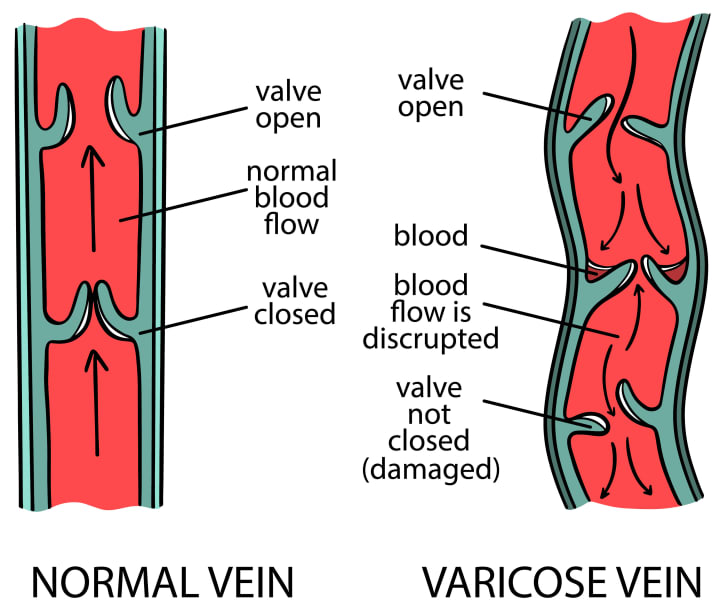
The Dynamic Duo: Estrogen and Progesterone
Estrogen and progesterone are the primary female sex hormones. They play a vital role in regulating the menstrual cycle, supporting pregnancy, and maintaining overall reproductive health. Additionally, these hormones influence blood vessel function by:
- Affecting the production of collagen and elastin, essential components of healthy blood vessel walls
- Modulating the smooth muscle cells lining the blood vessels, impacting vessel constriction and dilation
When hormonal imbalances occur, the integrity of blood vessels can be compromised, leading to the development of varicose veins.
Hormonal Changes and Varicose Veins: The Connection
Menstrual Cycle: Hormone levels fluctuate throughout the menstrual cycle, with estrogen levels peaking during ovulation and progesterone levels rising in the second half of the cycle. These fluctuations can lead to temporary vein dilation and increased susceptibility to varicosity.
Pregnancy: Pregnancy is a time of significant hormonal changes, with increased levels of estrogen and progesterone. The growing uterus also puts pressure on the pelvic veins, impeding blood flow and increasing the risk of varicose veins.
Menopause: The decline in estrogen and progesterone levels during menopause can weaken blood vessels and increase the likelihood of developing varicose veins.
Hormonal Contraceptives: A Double-Edged Sword
Hormonal contraceptives, such as birth control pills, patches, and injections, can help regulate menstrual cycles and prevent pregnancy but may also contribute to varicosity. These contraceptives often contain synthetic versions of estrogen and progesterone, which can affect blood vessel elasticity and strength.
Health Complications Associated with Varicose Veins
Varicose veins, while often viewed as a cosmetic issue, can lead to several health complications if left untreated. Some of these complications include:
Pain and discomfort: Varicose veins can cause aching, throbbing, or burning sensations in the affected area, particularly after long periods of standing or sitting. This discomfort can interfere with daily activities and reduce overall quality of life.

Swelling: The pooling of blood in varicose veins can cause the surrounding tissues to swell, leading to a condition called edema. This swelling can be particularly noticeable in the ankles and feet.
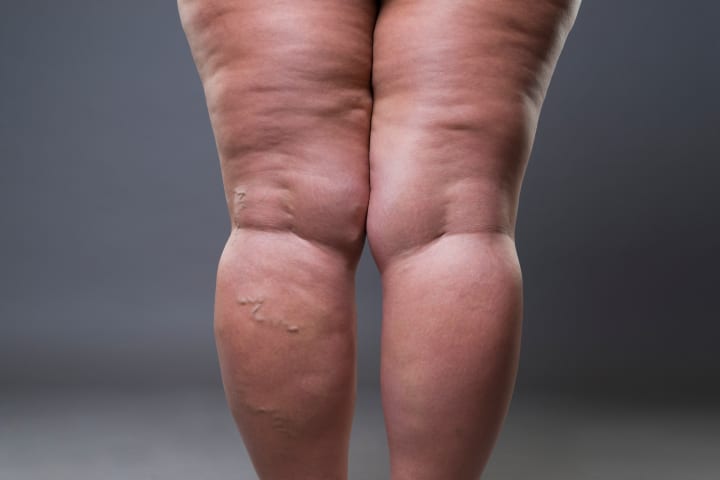
Skin changes: Varicose veins can affect the skin in the area, causing it to become dry, itchy, or discolored. In more severe cases, the skin may become inflamed, a condition known as stasis dermatitis, or develop ulcers due to poor blood circulation.
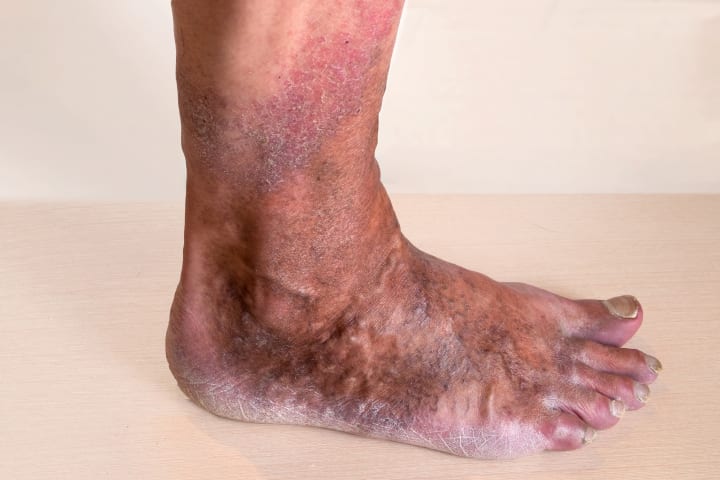
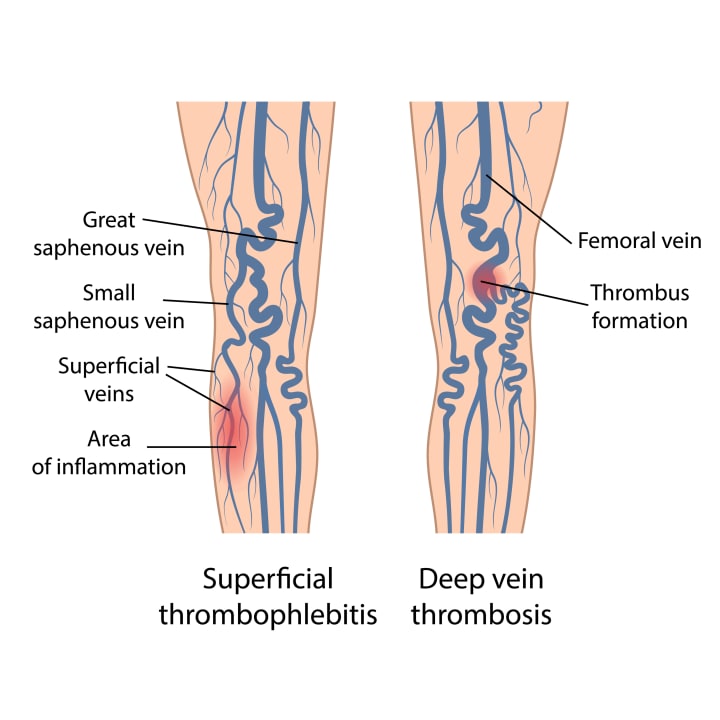
Superficial thrombophlebitis: This condition involves the formation of a blood clot in a superficial vein, causing inflammation, redness, and tenderness along the vein. While not typically life-threatening, superficial thrombophlebitis can be painful and may require treatment to alleviate symptoms.
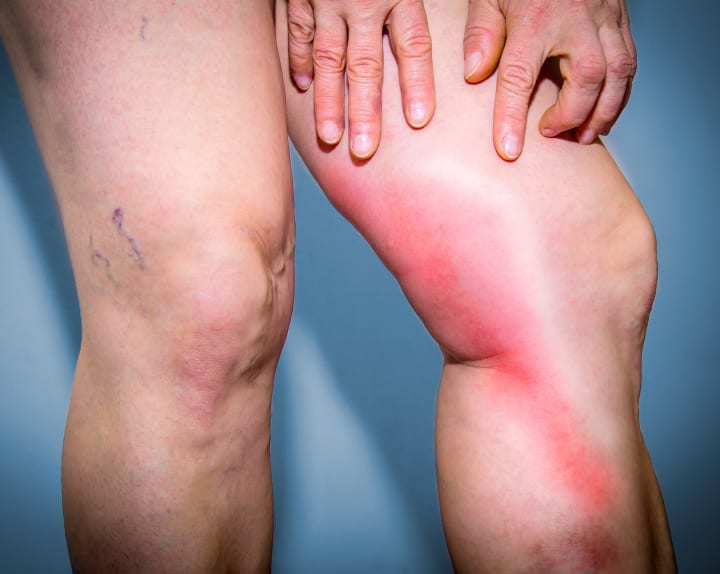
Deep vein thrombosis (DVT): Although rare, varicose veins can increase the risk of developing DVT, a more serious condition where a blood clot forms in a deep vein, usually in the legs. DVT can cause leg pain, swelling, and redness, and may lead to potentially life-threatening complications, such as a pulmonary embolism, if the clot dislodges and travels to the lungs.
Bleeding: In rare cases, the walls of varicose veins can become so thin and fragile that they rupture and bleed. This bleeding can be spontaneous or triggered by a minor injury. While the bleeding is usually not severe, it may require medical attention.
If you suspect that you have varicose veins or are experiencing any of these complications, it is essential to consult with a healthcare professional for proper assessment, diagnosis, and treatment options. Early intervention can help prevent the progression of varicose veins and reduce the risk of more severe complications.
About the Creator
Mohammad Barbati
Mohammad E. Barbati, MD, FEBVS, is a consultant vascular and endovascular surgeon at University Hospital RWTH Aachen. To date, he has authored several scientific publications and books regarding vascular and venous diseases.






Comments
There are no comments for this story
Be the first to respond and start the conversation.