The Day I Became Infertile
A postpartum story of gratitude, grief, and healing after a hysterectomy.
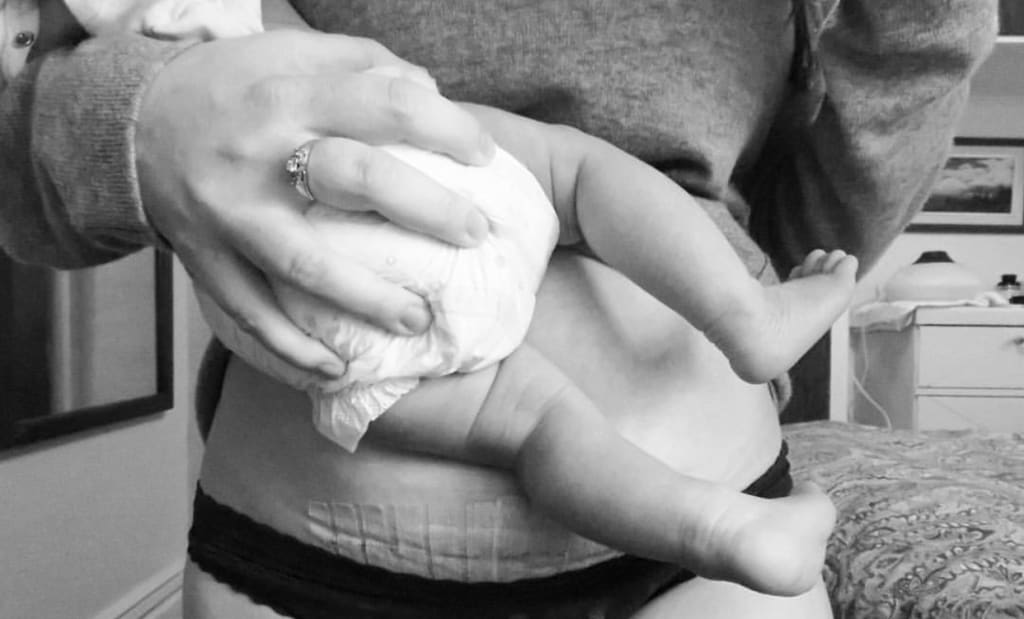
TW: This story involves a discussion of medical details such as bleeding, surgery, and infertility.
On November 11th, 2017, at 16 days postpartum, I had an emergency, life-saving hysterectomy. I had no warning signs, no symptoms, and no knowledge of just how serious postpartum complications are. My story is not an anomaly.
Rewind to the night before, around 11 PM: After over two weeks of normal postpartum healing, I passed a large blood clot about the size of a golf ball. After that, the bleeding stopped, and a quick Google search told me that this was okay—around two weeks postpartum the uterus often makes a big contraction, causing a temporary increase in bleeding. Regardless, I decided to play it safe and make a trip to the one Urgent Care center that was still open—only to be turned away because they didn’t take my insurance. Not yet worried and needing to care for my 13-month-old and newborn babies, I decided to go home, lie down, and monitor the bleeding on my own. I woke up around 2 AM, stood up, and felt another huge gush of blood. As I slowly walked the 30 feet to the bathroom, the blood clots continued to fall. Perhaps it was my overtired postpartum brain, but I still wasn’t worried—maybe this is what the internet meant by normal? I made myself believe everything was fine, and stood in the shower, blood running down my legs.
Just before 3 AM, it hit me: get yourself to the hospital. With no family nearby, I pumped a few bottles of milk for my newborn, left the babies with my husband, and drove myself to the hospital. I walked into the emergency center around 3 AM, and within five minutes they had sent me up to triage on the Labor and Delivery floor. By 4 AM, a dear friend came to take care of the babies, and my husband was able to join me at the hospital. I was bleeding uncontrollably, and my veins were collapsing as the medical team tried to run diagnostic tests. Two hours later, I was ready for surgery.
Around 6 AM the doctor decided to look for retained placenta. Still bleeding, they took me in for a D&C procedure, but the results were negative. At 7 AM the doctor sat down with my husband and me to suggest their next steps. I was getting weak from blood loss, and I was exhausted from the stress and anxiety of not knowing what was happening. I told them to do what they needed to do to make the bleeding stop, and the surgeon warned that the outcome could mean permanent infertility. My husband and I nodded to each other, and they took me back to the operating room. An hour and four blood transfusions later, it was over. I had lost the part of myself that carried my babies, the part that sustained the two perfect little lives I call my son and my daughter. I felt empty, grief-stricken, overwhelmed, and thankful to be alive. In the end, the doctor diagnosed me with placental site involution (PSI), which means that they don’t know what caused my spontaneous hemorrhaging.
This is what I took away from my experience:
- Listen to your body. Even if you’ve had children before and feel confident that you know what’s going on, if something feels off, just get it checked out—and don’t take no for an answer. The postpartum body needs time to heal, and if this healing is disrupted, you may not be aware of how to best handle complications on your own. After passing my first blood clot, I called my mom, who told me to go to the hospital right away. I didn’t feel the same sense of urgency she did, because I did not feel that my wellbeing was a priority. After a baby is born, they become your whole world, and it is easy to overlook your own needs. In my case, this lack of recognition could have cost me my life. New mothers need to be surrounded by people who help them help themselves; we cannot self-advocate if we do not allow ourselves to think of the “self.”
- Gratitude is a band-aid solution. I don’t know how many people told me that I should be thankful: to be alive, to have two beautiful children (one boy and one girl, they liked to point out), and to be able to move on with my life. Of course, that is all true, but telling someone to be grateful is also very dismissive of the feelings that are harder to process. Gratitude makes you feel guilty for leaning into the sadness, grief, and trauma, because the world is telling you how grateful you should be for what you have. I am still learning how to let myself feel these negative emotions. I am working to surround myself with people who I know will support both my gratitude and my grief, as part and parcel of the same journey.
I wrote this story in the hopes that it encourages other postpartum people to stay connected with their postpartum bodies, allow proper time to heal, and seek help at the first sign of any concern. Sometimes this means prioritizing ourselves over other important things. Sometimes it means we will have to advocate for ourselves, and it always means that we have the right to feel the full range of emotions that come with postpartum healing, and in my case, loss.






Comments
There are no comments for this story
Be the first to respond and start the conversation.